
FDA Approves iPhone Blood Glucose Monitor: Apple Watch Sugar Sensing Plan Advances
The fda just approved an iphone powered blood glucose monitor as apple watch sugar sensing plan continues – FDA Approves iPhone Blood Glucose Monitor: Apple Watch Sugar Sensing Plan Advances sets the stage for a future where managing diabetes is easier and more accessible than ever before. This groundbreaking approval marks a significant step forward in the fight against diabetes, bringing us closer to a world where continuous glucose monitoring is integrated into our daily lives.
The FDA’s approval of this iPhone-powered blood glucose monitor, coupled with Apple’s ongoing development of its Apple Watch sugar sensing technology, signifies a shift in diabetes care. This innovative approach promises to empower individuals with greater control over their health, providing them with real-time insights into their blood sugar levels.
The technology behind this breakthrough relies on non-invasive methods, eliminating the need for traditional finger-prick tests. This advancement has the potential to revolutionize diabetes management, offering a more convenient and less painful way for individuals to monitor their condition.
FDA Approval and its Significance
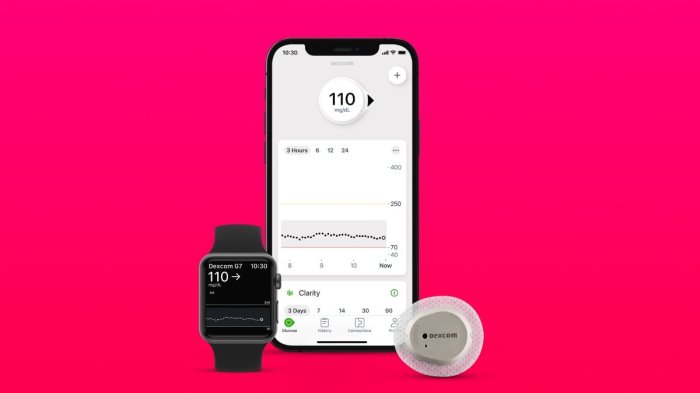
The FDA’s recent approval of an iPhone-powered blood glucose monitor marks a significant step forward in diabetes management. This innovative technology holds the potential to revolutionize how people with diabetes monitor their blood sugar levels, making the process more convenient, accessible, and user-friendly.
The FDA just approved an iPhone powered blood glucose monitor, a major step forward for diabetes management and another piece in Apple’s ongoing quest to integrate health tech into our lives. This brings us closer to the day when we can track our health metrics seamlessly, like we now manage our passwords with apps like authy vs google authenticator.
It’s exciting to think about how these innovations could lead to a future where managing chronic conditions becomes easier and more personalized, with technology playing a vital role in preventative care and overall well-being.
Impact on Diabetes Management
The approval of this device signifies a shift towards a more integrated and personalized approach to diabetes care. By integrating with the iPhone, the monitor provides a seamless and convenient way for individuals to track their blood sugar levels. This integration allows for real-time data sharing, enabling patients to make informed decisions about their diabetes management.
Benefits for Patients
The iPhone-powered blood glucose monitor offers numerous benefits for patients:
- Improved Convenience:The device eliminates the need for bulky and separate meters, making blood sugar monitoring more convenient and less intrusive.
- Enhanced Accuracy:The technology behind the monitor ensures accurate and reliable blood glucose readings, allowing for more precise diabetes management.
- Real-Time Data:The integration with the iPhone provides real-time data on blood sugar levels, empowering patients to make informed decisions about their diet, exercise, and medication.
- Improved Communication:The device allows for seamless communication with healthcare providers, enabling them to monitor progress and adjust treatment plans effectively.
Regulatory Process and Approval Criteria
The FDA’s approval process for medical devices is rigorous and ensures the safety and efficacy of the technology. The approval of the iPhone-powered blood glucose monitor involved a thorough evaluation of the device’s accuracy, reliability, and safety. The FDA considered various factors, including:
- Clinical Studies:The device underwent extensive clinical trials to assess its accuracy and performance in real-world settings.
- Safety and Efficacy:The FDA scrutinized the device’s design and functionality to ensure it meets the highest safety standards and provides accurate readings.
- User Interface:The FDA evaluated the device’s user interface to ensure it is user-friendly and intuitive, making it accessible to a wide range of individuals with diabetes.
Apple Watch Sugar Sensing Technology: The Fda Just Approved An Iphone Powered Blood Glucose Monitor As Apple Watch Sugar Sensing Plan Continues
The Apple Watch’s potential to monitor blood glucose levels non-invasively has generated immense excitement within the medical and technological communities. While the technology is still under development, Apple has made significant strides in its quest to create a convenient and reliable method for continuous glucose monitoring.
It’s exciting to see the FDA approve an iPhone-powered blood glucose monitor, bringing us closer to Apple Watch’s sugar sensing ambitions. But as we celebrate this leap forward, it’s also a reminder that technology is constantly evolving. Just last month, Apple declared the iPhone X “vintage,” alongside the original HomePod and AirPods ( still got an iphone x apple has just classed it as vintage alongside the original homepod and airpods ).
While this might seem like a small detail, it underscores the rapid pace of innovation in the tech world. It’s a reminder that even cutting-edge devices can quickly become outdated, and that the future of health monitoring, like the iPhone-powered glucose monitor, is constantly being shaped by new developments.
The Technology Behind Apple Watch Sugar Sensing
Apple’s approach to non-invasive blood glucose monitoring relies on a combination of advanced technologies, including optical sensors and machine learning algorithms. The watch utilizes a specialized sensor that emits near-infrared light through the skin. This light interacts with the interstitial fluid, which contains glucose, and the sensor measures the amount of light that is reflected back.
By analyzing the changes in light absorption and reflection, the sensor can estimate the glucose concentration in the interstitial fluid.
The FDA’s recent approval of an iPhone-powered blood glucose monitor is a huge step forward for Apple’s health initiatives. This move, coupled with the ongoing development of Apple Watch sugar sensing, suggests Apple is committed to making its devices even more integrated into our health journeys.
It’s interesting to note that Apple recently purchased the domain “iworkai.com,” fueling speculation about a major AI overhaul for its iWork apps. Perhaps this AI push could even play a role in enhancing Apple’s health tech, making blood sugar monitoring even more personalized and predictive.
Methods for Measuring Blood Glucose Levels Non-Invasively
- Optical Sensors:The Apple Watch’s primary method involves using near-infrared light to measure glucose levels in the interstitial fluid. This approach is based on the principle that different substances absorb light differently. By analyzing the pattern of light absorption and reflection, the sensor can estimate the glucose concentration.
- Machine Learning Algorithms:The data collected by the optical sensors is then processed by machine learning algorithms. These algorithms have been trained on large datasets of blood glucose readings from individuals with diabetes. This training allows the algorithms to identify patterns and correlations in the sensor data, enabling them to accurately predict blood glucose levels.
Comparison with Traditional Blood Glucose Monitoring Methods
- Traditional Methods:Traditional blood glucose monitoring methods typically involve pricking the finger to obtain a blood sample. This method is invasive and can be painful, especially for individuals who require frequent blood glucose monitoring.
- Apple Watch Technology:The Apple Watch’s non-invasive approach offers a potentially more convenient and comfortable alternative to traditional methods. By eliminating the need for finger pricks, it can improve the user experience and encourage more frequent blood glucose monitoring, leading to better diabetes management.
Impact on Diabetes Care and Management
The FDA approval of an iPhone-powered blood glucose monitor marks a significant milestone in diabetes care, paving the way for more convenient and accessible monitoring. This technology holds the potential to revolutionize how individuals with diabetes manage their condition, impacting patients, healthcare providers, and the healthcare system as a whole.
Potential Benefits for Patients, The fda just approved an iphone powered blood glucose monitor as apple watch sugar sensing plan continues
The availability of a convenient, user-friendly blood glucose monitor integrated with a smartphone can significantly benefit patients with diabetes. This technology offers several advantages:
- Increased Frequency of Monitoring:The ease of use and portability of the device could encourage patients to monitor their blood glucose levels more frequently, leading to better control of their blood sugar levels.
- Improved Data Management:Data from the monitor can be seamlessly integrated with smartphone apps, providing patients with a comprehensive overview of their blood sugar trends over time. This can help patients identify patterns and make informed decisions about their diabetes management.
- Enhanced Patient Engagement:The user-friendly interface and accessibility of the data can empower patients to take a more active role in managing their diabetes. This can lead to increased adherence to treatment plans and improved self-management skills.
- Reduced Stigma:The discreet nature of the technology could help reduce the stigma associated with diabetes, allowing individuals to manage their condition more comfortably in public settings.
Potential Benefits for Healthcare Providers
The availability of real-time blood glucose data can also benefit healthcare providers, enabling them to provide more personalized and effective care:
- Improved Patient Monitoring:Healthcare providers can access patient blood glucose data remotely, allowing for more frequent and comprehensive monitoring. This can help identify potential complications early and adjust treatment plans promptly.
- Enhanced Communication:The technology can facilitate better communication between patients and healthcare providers, allowing for timely sharing of blood glucose data and discussions about treatment strategies.
- Data-Driven Decision Making:Real-time data can provide healthcare providers with valuable insights into patient blood sugar patterns, enabling them to make more informed decisions about treatment adjustments and interventions.
Potential Benefits for the Healthcare System
The widespread adoption of this technology could also benefit the healthcare system as a whole:
- Reduced Healthcare Costs:Improved diabetes management through more frequent monitoring and early intervention can lead to a reduction in complications and hospitalizations, potentially reducing healthcare costs in the long run.
- Increased Efficiency:The ability to access patient blood glucose data remotely can streamline healthcare processes and reduce the need for in-person appointments.
- Improved Outcomes:Better diabetes management through technology can lead to improved patient outcomes, including reduced risk of complications and improved quality of life.
Challenges and Limitations
While the potential benefits of this technology are significant, it is important to acknowledge potential challenges and limitations:
- Accuracy and Reliability:The accuracy and reliability of the technology need to be rigorously tested and validated to ensure it provides accurate blood glucose readings.
- Accessibility and Affordability:The technology needs to be accessible and affordable for all individuals with diabetes, regardless of their socioeconomic status.
- Data Privacy and Security:Robust measures need to be in place to protect patient data privacy and security, ensuring that sensitive information is not compromised.
- Integration with Existing Systems:The technology needs to seamlessly integrate with existing healthcare systems and electronic health records to facilitate data sharing and improve interoperability.
- Training and Support:Patients and healthcare providers need adequate training and support to effectively use and interpret the data generated by the technology.
Future of Continuous Glucose Monitoring

The recent FDA approval of an iPhone-powered blood glucose monitor and the ongoing development of Apple Watch sugar sensing technology signal a new era in diabetes management. Continuous glucose monitoring (CGM) is poised to revolutionize how individuals with diabetes track and manage their blood sugar levels, offering unprecedented convenience and insights into their health.
This technology has the potential to significantly improve diabetes care and management, leading to better outcomes for individuals and a more efficient healthcare system.
Timeline for the Future Development and Adoption of Continuous Glucose Monitoring Technologies
The advancement and adoption of CGM technology is expected to follow a trajectory of continuous innovation and increasing accessibility. Here’s a possible timeline for the future development and adoption of CGM technologies:
- Near Future (2023-2025):Improved accuracy, smaller form factor, and increased integration with existing smart devices will be key priorities. The focus will be on making CGM technology more user-friendly and accessible to a wider range of individuals. We can expect to see more affordable options and greater compatibility with various mobile devices.
- Mid-Term (2026-2030):Advancements in sensor technology will lead to longer wear times, potentially extending to weeks or even months. Non-invasive CGM technologies, such as those utilizing optical or acoustic methods, will gain traction, offering a more comfortable and convenient experience. Additionally, AI and machine learning algorithms will be incorporated into CGM systems, providing personalized insights and predictive capabilities for blood sugar management.
- Long-Term (2031 onwards):The integration of CGM technology into closed-loop systems will become more prevalent. These systems will automatically adjust insulin delivery based on real-time blood sugar readings, reducing the burden of manual adjustments for individuals with type 1 diabetes. The development of personalized CGM solutions, tailored to individual needs and preferences, will become increasingly important.
Potential Impact of Continuous Glucose Monitoring Technology on Individuals and Society
Imagine a future where individuals with diabetes can effortlessly track their blood sugar levels throughout the day, receiving real-time alerts and personalized recommendations for managing their health. This is the potential impact of CGM technology on individuals and society.
“CGM technology has the potential to empower individuals with diabetes to take control of their health and live healthier lives.”
Here’s a hypothetical scenario showcasing the potential impact of this technology:
- Individual Impact:Sarah, a 25-year-old with type 1 diabetes, wears a discreet CGM sensor that continuously monitors her blood sugar levels. The data is automatically transmitted to her smartphone, providing her with real-time insights into her blood sugar fluctuations. Sarah receives personalized alerts when her blood sugar levels are too high or too low, allowing her to adjust her insulin dosage and diet accordingly.
The CGM data also helps her identify patterns in her blood sugar levels, enabling her to make proactive lifestyle changes to improve her overall health.
- Societal Impact:As CGM technology becomes more widespread, the burden of diabetes management shifts from individuals to the healthcare system. With real-time data, healthcare professionals can remotely monitor their patients’ blood sugar levels, enabling early intervention and reducing the risk of complications.
The cost of diabetes management is expected to decrease as individuals can avoid costly hospital visits and emergency room visits. Furthermore, the increased awareness of blood sugar management fostered by CGM technology can lead to a more informed and proactive approach to diabetes prevention and overall health.
Potential Advancements in Continuous Glucose Monitoring Technology
The future of CGM technology holds exciting possibilities for advancements that will further enhance its capabilities and impact.
- Non-invasive CGM:Current CGM technologies require invasive procedures to insert sensors under the skin. Non-invasive methods, such as optical or acoustic sensing, are being actively researched and developed. These technologies promise a more comfortable and convenient experience for users.
- Improved Accuracy and Precision:Advancements in sensor technology and data analysis algorithms will lead to more accurate and precise blood sugar readings. This will enable individuals to make more informed decisions about their diabetes management.
- Longer Wear Times:Current CGM sensors typically need to be replaced every few days. Future sensors will be designed to last for weeks or even months, reducing the frequency of insertions and improving user convenience.
- Integration with Closed-Loop Systems:The integration of CGM technology with closed-loop systems will enable automated insulin delivery based on real-time blood sugar readings. This will significantly reduce the burden of manual insulin adjustments for individuals with type 1 diabetes.
- Personalized CGM Solutions:The development of personalized CGM solutions, tailored to individual needs and preferences, will become increasingly important. This will ensure that individuals receive the most relevant and helpful insights from their CGM data.
Ethical Considerations
The integration of personal devices like smartphones and smartwatches into healthcare monitoring raises crucial ethical considerations that must be addressed to ensure responsible and equitable use of these technologies.
Data Privacy and Security
The potential risks and benefits of data privacy and security in the context of using personal devices for healthcare monitoring are multifaceted. On the one hand, the collection and storage of sensitive health data raise concerns about potential breaches and unauthorized access.
On the other hand, secure and responsible data management can enable personalized healthcare and improved patient outcomes.
- Data Security:The use of personal devices for healthcare monitoring introduces potential vulnerabilities for data breaches. Secure data encryption, authentication protocols, and robust cybersecurity measures are crucial to protect sensitive health information from unauthorized access.
- Data Privacy:The ownership and control of health data generated by personal devices is a complex issue. Clear guidelines and regulations are needed to define data ownership, consent for data sharing, and the purpose for which data can be used.
- Data Sharing:Data sharing between patients, healthcare providers, and researchers can be beneficial for improving healthcare outcomes. However, it is essential to ensure that data sharing occurs with informed consent and appropriate safeguards to protect patient privacy.
Impact on Healthcare Access and Equity
The potential impact on healthcare access and equity is a critical aspect of integrating personal devices into healthcare. While these technologies have the potential to improve access to healthcare, they also raise concerns about exacerbating existing health disparities.
- Digital Divide:Access to smartphones and smartwatches is not universal, potentially excluding individuals from benefiting from these technologies. This digital divide can exacerbate existing health disparities based on socioeconomic status, location, and other factors.
- Accessibility:The user interface and functionality of personal devices need to be accessible to individuals with disabilities, ensuring equitable access to healthcare monitoring.
- Cost:The cost of personal devices and associated healthcare services can create barriers to access, particularly for individuals with limited financial resources.







